Taxonomy
In the classical classification, scoliosis is mainly classified according to the age of onset of scoliosis.
Accordingly; 0-3 years of age are called ‘Infantile Scoliosis’, 4-10 years of age are called ‘Juvenile Scoliosis’, and those who are 11 years and older are called ‘Adolescent Scoliosis’.
In recent years, in addition to this classical classification, a new classification has been developed as Early Onset and Late Onset. Early Onset Scoliosis includes 10 years of age and below, and Late Onset Scoliosis includes 11 years of age and above.
The logic of this new classification is actually due to the difference in approach to the treatment of scoliosis in these two age groups.
The spine tends to grow in patients under the age of 10, and the surgical treatments during this period are procedures aimed at orienting the spine during growth rather than freezing it. For this reason, these procedures are called ‘Growth Friendly Surgeries’.
At the age of 11 and above, the spine has largely completed its growth and bone freezing (fusion) surgeries are preferred.
Degree of Curvature
Scoliosis, in plain terms, is the tilt of the spine sideways when viewed from the opposite side.
Deviations up to 10 degrees are considered asymmetry, not scoliosis, and do not require any follow-up or treatment.
In scoliosis between 10-20 degrees, if the patient is under the age of 10, follow up at regular intervals is useful.
Corset therapy is appropriate for patients who are between 20-40 degrees and whose height continues to grow, that is, for patients with growth potential.
If it is over 40 degrees, surgical treatment is performed.
These are simple generalizations given to you for information purposes.
Normally, each scoliosis is evaluated on a patient-specific basis and the treatment method is chosen individually.
Early-onset Scoliosis was divided into 5 groups as Idiopathic, Congenital, Thoracogenic, Neuromuscular and Syndromic by the Scoliosis Research Society in 2015.
In this article, you will be given information about the most common type, idiopathic scoliosis, the causes of which is unclear.
Although under 10 years old will be grouped as Early Onset Scoliosis, Infantile (0-3 years old) and Juvenile (4-10 years old) scoliosis titles will continue to be used for ease of expression.
Idiopathic Scoliosis
1-3% of all idiopathic scolioses are infantile and 12-21% are juvenile scoliosis.
Infantile scoliosis is more common in boys (3 times more than girls). In general, before the age of 1, the family notices the asymmetry on the baby’s back and the diagnosis is made.
The juvenile type is more common in girls (3 times more than boys). Generally, boys are diagnosed around the age of 5, and girls around the age of 7.
Early Onset Scoliosis
When the physician encounters an early-onset scoliosis, firstly, a detailed history is taken.
The presence of additional diseases must be investigated. Because if there is another disease that causes scoliosis (Neuromuscular scoliosis, Syringomyelia, Spinal tumor, Congenital spinal deformity, Other intraspinal anomalies, Neurofibromatosis, Syndromic disorders, Spinal infection etc.), the treatment is completely different, that is, primarily planned by considering this disease. For this purpose, the physician should question all the details.
Especially the pregnancy history of the mother is important. Health problems of the mother during pregnancy, previous pregnancies, medications used, duration of pregnancy, method of delivery (vaginal or cesarean section) and weight gain are questioned.
For example, infantile scoliosis rate is higher in breech presentations or premature births.
Cognitive functions should also be examined, because 13% of premature children with infantile scoliosis are accompanied by mental retardation.
Another warning finding for infantile scoliosis is plagiocephaly, that is, the image disorder that occurs with the flattening of certain parts of the baby’s head. It has been observed in the literature that plagiocephaly accompanies all children with infantile scoliosis.
Physical examination involves some difficulties in young children. Because there is a problem of adaptation, the bone structures are not fully developed yet, and motor or sensory neurological examination is more difficult.
Therefore, careful observation in physical examination is very important. Presence of pathological findings is sought in posture, asymmetry (head, shoulder, torso or pelvic asymmetry) and forward bending tests. Chest or abdominal asymmetry and limitation of chest movements are especially suspicious for Syndromic Scoliosis. Anomalies in the neurological evaluation, difference in length between the legs, one leg being thinner than the other, and foot deformities are findings that may accompany scoliosis, so they should be alerting in the physical examination.
One of the most common conditions associated with infantile scoliosis is hip dislocation. Hip dislocation, which is called Developmental Dysplasia of the Hip (DDH) in medical terminology, is 10 times more common in infantile scoliosis compared to the normal population and is more common especially in girls.
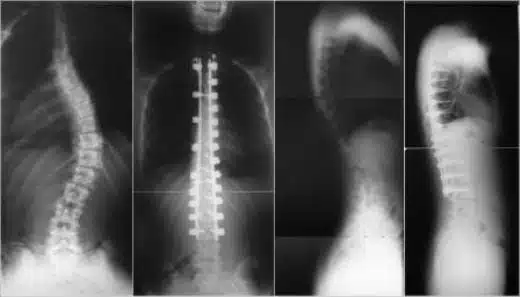
Scoliosis Radiographies
The scoliosis is diagnosed mainly by radiology.
The size and type of scoliosis are determined by scoliosis radiographs taken from the front and the side, and the presence of other accompanying pathologies is revealed. These radiographs must also include the cervical (neck) spine and pelvis, that is, the hip joints. Some measurements made on the x-ray give information about the tendency of the curvature to progress.
It is also important in terms of documentation, that is, to track whether scoliosis increases in follow-ups.
Advanced radiological examinations are not routinely performed in every Early Onset Scoliosis.
You can review when an MRI should be required in scoliosis patients from the article HERE.
Progression
90% of infantile idiopathic scoliosis disappear by themselves, while 10% continue to progress.
The point to be noted here is; these rates are valid for idiopathic scoliosis, that is, for scoliosis of which the cause is unknown, in other words, there is no underlying disease. E.g.; If scoliosis is caused by a congenital anomaly or a neuromuscular disease, it will continue to progress.
There are also some criteria to predict which curvatures tend to progress in idiopathic scoliosis.
Your doctor will inform you about this after the examination and measurements on the x-rays.
As a general rule, earlier scoliosis tends to heal more spontaneously than later scoliosis.
Unfortunately, the results are malignant in untreated and advanced infantile scoliosis. More than half of patients will have scoliosis greater than 70 degrees by the age of 5 years.
The critical point here is lung development. Because the deterioration of the evolvement of the rib cage due to scoliosis that developed at an early age causes the Thoracic Insufficiency Syndrome, which is characterized by small lung volume and impaired pulmonary functions.
Juvenile idiopathic scoliosis progresses more slowly than the infantile group. Curvatures that occur at an early age are more progressive.
The rate of the curve determines the prognosis; the scoliosis process is slower in curves below 25 degrees, and faster in curves above 25 degrees.