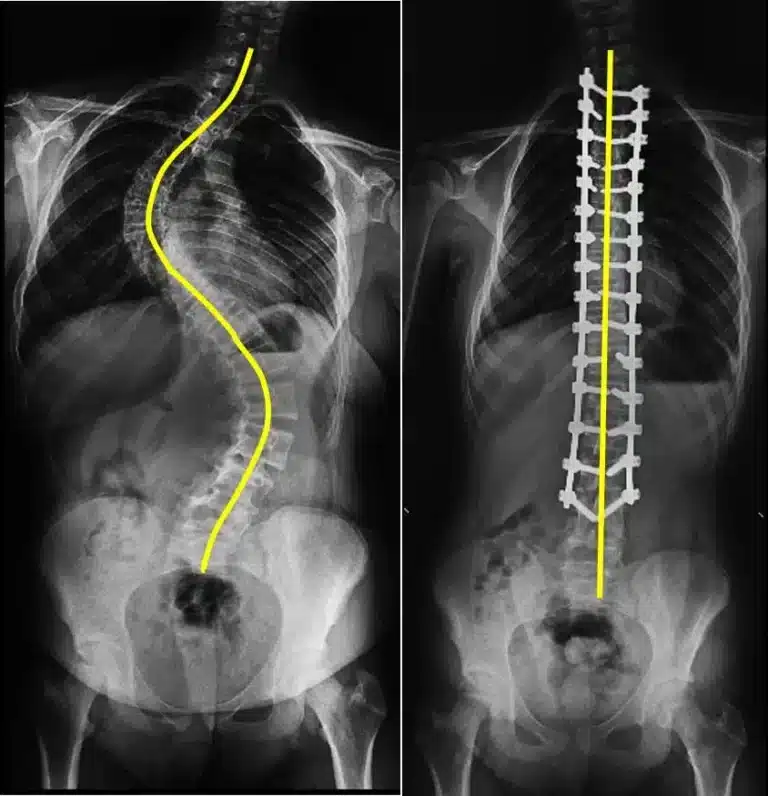
After the decision of surgery for scoliosis is made, the thing that patients and their relatives are most curious about is the method to be chosen in the surgery.
The first thing to say here is that each surgical method is specific to the patient.
In other words, many factors such as the patient’s age, the type of scoliosis (See Scoliosis Classification), the size of the curvature, and co-morbid diseases affect the details and technique of the scoliosis surgery to be performed.
For example, in congenital scoliosis, the aim is to surgically eliminate the bone or neural anomalies that cause scoliosis, while in idiopathic scoliosis, the main purpose is fusion, that is, freezing the vertebrae in the appropriate position.
Your doctor will give you detailed information about the surgery to be performed.
The aim of this article is to give you general information about what is done in a scoliosis surgery.
The purpose of fusion, that is, knitting the bones together, is to ensure the continuation of the corrected curvature. Because especially during the growth period, the spine tends to continue to bend due to the nature of the scoliosis disease.
In other words, when fusion cannot be achieved, the improvement obtained during the surgery will be lost. This tendency of the spine, which is caused by scoliosis, decreases after the skeletal development is completed, that is, after an average of 18 years of age.
Therefore, the progression of the curvature is slower in adult scoliosis and its treatment is different.
Because the spine is no longer flexible in adults and correction surgeries require some specific procedures and maneuvers.
Growth-friendly Methods
In recent years, a new method called ‘stretching method’ (vertebral body tethering) has started to be applied as an alternative to correct scoliosis without fusion in growing children.
In this technique, screws are inserted from the side by entering the convex side of the curvature in the back or waist through endoscopy or mini portals, and the curvature is corrected by stretching these screws with a thick thread.
The goal here is not to completely correct the curvature but to stop growth on the convex side. The spines will now only shape on the concave side of the curvature. This way, as the child grows, the curvature in the spine will correct itself. When the patient reaches adult age, the spine will lose its flexibility, the tendency to bend to the side will decrease, so it will remain in its reformed state.
The advantage of this method is that the movement of the spine will continue since the bone freezing(fusion) is not performed. The key factor for the stretching method is that the child will continue to grow.
The effectiveness of this method is much less in children who have completed the rapid growth period, that is, the adolescence period.
Neuromonitorization and Cell-Saver
Fusion surgeries are performed by placing screws from the back of the spine. Correction of curvature is ensured by placing rods shaped in the appropriate position on these screws.
During the surgery, the spinal cord itself and the proceeded nerves are controlled by the Neuromonitorization process, so that possible nerve injuries can be prevented or necessary interventions can be made for the injury. The use of neuromonitoring has greatly reduced the rate of nerve damage from spinal surgeries.
The blood collected at the surgical field during the surgery is passed through special filters in the device called Cell Saver and returned to the patient.
Thus, the patient’s own blood is used and there is no need to give blood externally.
Does Fusion of the Spines Restrict Movement?
After the curvature is corrected by means of screws and rods, the bones taken from the patient (autogenous) and obtained from other people (allogeneic) are placed on the vertebrae to which the screws are applied, so that union can be achieved.
Dorsal Vertebra
One of the most frequently asked questions about this surgery is the disadvantages of fusing the vertebrae together and losing their mobility.
The most common type of scoliosis is idiopathic, and in the idiopathic type, the curvature is mostly in the spine in the back.
The dorsal vertebrae are attached to the ribs, and they, in turn, join circularly with the vertebrae posteriorly and the sternum anteriorly to form the rib cage. Because of this connection, there is very little movement in the back spines, and freezing(fusion) these spines with scoliosis surgery almost does not affect the normal daily activities of the patient.
Lumbar Vertebra
Unlikely, lumbar spines do not have such a connection and are more mobile. For this reason, many studies have been published in the medical literature for years to maintain mobility by including less of the lumbar vertebrae in fusion.
While planning the operation, as few of the lumbar spines as possible tried to be included.
But the following point should not be forgotten; If the curvature involves the lumbar vertebrae and fusion is not performed because of the concern of loss of motion while it should have been included, the body may continue to bend through these remaining mobile vertebrae. This situation leads to serious balance and posture disorders after surgery. Because, since the spines in the back are surgically frozen, they can no longer adapt to compensate for the bending in the lumbar vertebrae.
Spine surgeons already take this into account when planning surgery.
The aim is to achieve the best result by freezing(fusion) the spine as little as possible to recover the curvature.
Implants
Screws and rods used during surgery are titanium alloys.
They do not cause an allergic reaction in the body.
They can be detected only by very sensitive metal detectors.
Once the union(fusion) is succeeded, these implants are no longer needed.
However, this does not mean that the implants will be removed after fusion. Implants remain in the patient’s body for life unless there is a problem that requires removal.