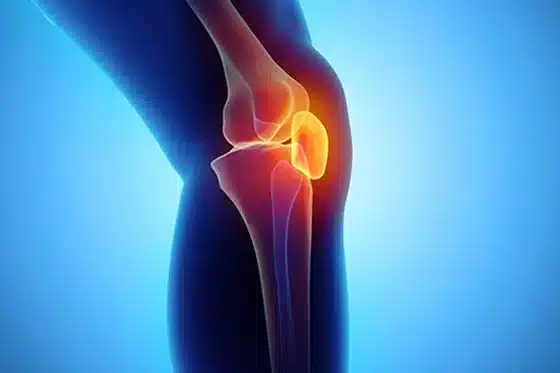
The knee joint is the largest joint in our body. The three bones that make up this joint are the femur (thigh), tibia and patella (knee cap), which are tightly held together by ligaments and muscles. The proper movement of the joint and the ability to carry the load of our body depend on the strength of all the structures that make up the joint and their functioning in harmony. The structures most frequently exposed to knee injuries are menisci, cruciate ligaments, lateral ligaments and cartilage surface.
What is Meniscus?
Menisci are crescent-shaped pieces of cartilage that act as shock absorbers between femur and tibia. Each knee has two menisci; the inner and outer meniscus. It is rigid and at the same time elastic. By acting as a buffer, they help the joint to remain stable under load. Meniscus, which fills the inside of the joint like a pillow to increase the bearing surface, ensures the proper functioning of the knee joint during our daily activities.
Why does Meniscus Tear?
Meniscus tears can occur for a variety of reasons, usually as a result of rotation or sprain of the knee. They are often torn, squeezing between thigh and tibia, when the foot does not rotate but the body does, during weight lifting and sports activities. In addition, meniscus tears may appear due to wear as a part of calcification in advanced ages.
What are the Complaints of Meniscus Tear?
The patient feels pain in the knee, relative on the location of the tear. In addition, limitation of movement or locking of the knee may occur due to the interference of the torn piece during joint movement. Severe pain may be felt during the rupture, which may be accompanied by swelling in the knee due to fluid accumulation in the joint. Your doctor may reveal this pain by performing some tests that compress the meniscus during the physical examination. These tests are important to understand whether the pain is really coming from the meniscus. In the next step, the tear is visualized by MRI and the diagnosis is confirmed.
Treatment of Meniscal Tears
Treatment of meniscus tear is divided into conservative (non-surgical) and surgical treatments. In conservative treatment, physiotherapy, rest, knee protection, PRP and stem cell injections can be performed. Meniscus surgeries are performed with closed method in today’s technology. In this method, which we call arthroscopic surgery, the knee joint is entered through two holes, the inside of the knee joint is viewed and examined with a video camera thinner than a pencil.
By entering the other hole with special tools, the meniscus tear is sutured or the torn part is removed, depending on its type. In this surgery, which is performed without any bleeding, these two holes are closed with a stitch.
What is Arthroscopy?
Arthroscopy is a method used in injuries of intra-articular structures or cartilage in the shoulder, ankle, wrist, elbow and hip joints, most commonly in the knee joint. The most significant advantage is that the joint is not opened and the procedure is performed completely closed. Thus, both comfortable access to the structures in the joint is ensured, and the surgery is completed without bleeding or damaging any other structure.
How is Arthroscopic Surgery Performed?
Knee arthroscopy is the most preferred application for intra-knee injuries. The surgery is performed using a camera and application tools through two 1 cm holes drilled on both sides of the knee joint. Initially, the knee joint is filled with fluid to obtain a clear view within the joint. All structures in the joint are then displayed and possible problems are detected. Necessary repairs are performed in damaged areas. The average operation time is half an hour. Unless there is a special reason, all surgeries are performed without general anesthesia, by anesthetizing the patient only from the waist down. Compared to open surgeries, the wound is very small and the infection rate is much lower.
After Arthroscopic Surgery
Knee arthroscopy is a closed surgery. So, the patient can get up early. In general, after arthroscopy, if no serious operation has been performed on the bone and cartilage, the patient is discharged on the same day. This is possible in meniscus repairs, surgeries where meniscus tears are removed, or ligament surgeries.
Depending on the degree of the operation performed, restrictions may be required to load the joint. After meniscus surgeries, in most cases, the patient can walk immediately with weight bearing. In anterior cruciate ligament surgeries, weight bearing can be delayed a little longer. In the repair of bone cartilage lesions, full weight-bearing is not performed for an average of one and a half months. Because the cartilage tissue that is repaired or replaced after the procedure is expected to heal completely.
Pain is much less common in closed surgeries than in open ones. Regaining range of motion and strengthening of the muscles around the joint happen in a much shorter time with physiotherapy, and the patient can return to his daily life in a much shorter time.
What is Anterior Cruciate Ligament?
The anterior cruciate ligament is a very important structure that connects the femur (thigh) and tibia bones in the knee joint and is responsible for the stability of the knee in the anterior-posterior direction. Anatomically, it extends from the inner side of the knee joint to the outer side and from the front to the back. It ensures the stability of the knee during the opening and closing movements as well as sliding back and forth movements of the knee, and prevents the joint from making abnormal movements and, consequently, injury. It is about 3 cm long and 1 cm thick. It usually breaks off during sports activities or after traumas at a young age. The patient may hear a sound at the moment of this rupture. When the anterior cruciate ligament ruptures, the normal movement mechanics of the knee are disrupted, and the resulting abnormal movements cause both pain and deterioration of the articular cartilage over time. In addition, this situation sets the stage for the rupture or breaking of other structures (eg meniscus) in the knee joint.
Symptoms of Anterior Cruciate Ligament Injuries
- During the trauma, there is a breaking sound from the knee.
- Severe pain is felt locally in the knee region and in the entire leg.
- Swelling, bruising or redness may occur in the knee due to bleeding inside the joint.
- The fluid accumulated in the knee reduces the mobility of the joint, there is difficulty in opening and closing the knee or pressing on it, the patient can walk with a limp or with crutches.
- During walking, a sudden emptiness or a feeling of stepping into the void occurs in the knee, which is a typical finding of injuries.
- In some cases, a feeling of dislocation, in which the knee moves from its place, occur.
Reconstruction of Anterior Cruciate Ligament
Some factors are taken into account in determining the treatment after anterior cruciate ligament rupture. If the ligament is completely ruptured radiologically and during the examination it is detected that the tibia moves forward abnormally under the femur (instability), ligament repair should be considered. Anterior cruciate ligament repair is actually a replacement surgery. The procedure is performed with arthroscopy, that is, closed. First of all, the remnants of the torn ligament are cleaned, and if any, other damaged structures in the knee joint are repaired. Then, two tendons in the inner-posterior part of the knee joint are taken and prepared. The removed tendons are folded in half on themselves and a 4-fold ligament is obtained. This 4-fold ligament is up to 30% stronger than the normal anterior cruciate ligament. In this way, the knee can regain stable function after surgery. This new ligament is inserted into the thigh and tibia through the tunnels opened in accordance with the original and locked. The entire process is carried out closed and lasts about 1 hour.
After Anterior Cruciate Ligament Surgery
Unless there is a special reason, all surgeries are performed without general anesthesia, by anesthetizing the patient from the waist down. The aim here is to avoid the difficulties of general anesthesia and to bypass the operation process as easily as possible. Therefore, the patient may need to stay in the hospital for 1 night after the operation. On the first day of the surgery, the patient can stand up with a full load. In order for the anterior cruciate ligament repair surgery to be successful, the physiotherapy to be applied after the operation is also very important. Physiotherapy is continued immediately after the operation, starting with simple exercises and gradually increasing them. The physical therapy process varies according to the patient’s activity level and expectations before the surgery. For example, a much more intense program is applied to enable athletes to return to training again.
Why Does Cartilage Damage Occur in the Knee?
The knee joint consists of smooth cartilage surfaces that can slide over each other. The entire joint cavity is covered from the inside by a membrane called the synovium. The joint capsule, on the other hand, protects the joint from the outside by wrapping it all around. Menisci, cruciate and lateral ligaments are the structures that provide the stability of the knee located in the joint during movements. The ability to perform activities such as walking, running, squatting and getting up without any problems depends on the harmony of these structures that make up the joint. Cartilage damage can occur either directly with the blows on the cartilage or indirectly due to abnormal movements that occur due to damage to one of the structures in the joint. Cartilage is not a self-renewing tissue. The small scratches and cracks that form will deepen gradually under the load over time. As the cartilage tissue disappears, the load carrying capacity of the joint begins to decrease and pain occurs.
Treatment of Cartilage Damage in the Knee
Cartilage damage in the knee joint can be divided into two groups as mild and severe level damage. The treatment method in mild damage is to stay away from activities that will force the joint, and to strengthen the muscles around the joint with weight loss and physiotherapy. Because when these muscles are weak, abnormal movements of the joint cannot be prevented and the cartilage damage progresses faster. Some medications may also be required for pain management. In patients who do not benefit from these treatments, the next step is injections into the knee (PRP and Stem cells). The aim here is to stop the progression of the damage and help the healing process. If the damage and the cartilage loss area is large, surgical treatments (micro-fracture method, mosaicplasty and cartilage transplantation) are on the agenda.
What is PRP?
PRP therapy, which has been increasingly used in cases such as knee calcification, cartilage and ligament injuries, and shoulder muscle rupture in recent years, is actually a method prepared from the person’s own blood and therefore does not fall into the category of drugs. The process begins with the acquisition of serum within the concentration of coagulation cells in the blood. This process takes about half an hour after taking blood. The aim is to deliver this serum, which is full of growth and healing factors, directly to the damaged area in the joint. Here, the following question may come to mind: Why do not these factors that already exist in the blood do the healing work, and we give them from the outside? Because the blood supply of the damaged tissues is impaired, so these factors cannot reach the area because there is not enough blood reaching that area. With PRP injection, serum filled with these factors is delivered directly to the field.
What is Stem Cells Therapy?
In recent years, stem cell applications have also been used with the opportunities created by technological developments. With stem cell methods proven by scientific studies and approved by the Ministry of Health, good results can be achieved without surgery, especially in knee problems. Stem cell collection is performed with a simple procedure from the fatty area of the abdomen or the pelvis. However, since the procedure is painful, it is appropriate to perform it under mild sedation (anesthesia). Then, the stem cells isolated by special processes are injected into the joint either freshly at the same time or after they are reproduced in the laboratory environment. Stem cell means a cell that can transform into any type of cell in the body, according to the need. The aim here is that these stem cells become healing cells, stopping the cartilage damage process and even aiding healing.
Microfracture Method
It is a method applied in limited cartilage injuries smaller than 3 cm. After the damaged area is cleaned of cartilage residues, holes a few mm deep extending into the bone are drilled at 5 mm intervals. In this way, a path is set for stem cells in the bone marrow to reach the damaged area through these holes. Stem cells that settle into the blood clot formed in the damaged area have the ability to transform into cartilage-like cells when the appropriate environment is provided. In recent years, roof implants called matrix have been developed so that this clot can better adhere to the damaged area and organize. These membrane-shaped tissues, mostly made of collagen, can be adhered to the damaged area after the microfracture is performed. Until new cartilage-like tissue is formed, it is necessary to protect the joint from loading by using crutches for six to eight weeks postoperatively. Similarly, for the formation of this cartilage repair tissue, it is necessary to move the joint slowly and in a controlled manner and perform slight exercises for a few weeks in the postoperative period.
Mosaicplasty
It is the process of taking cylindrical pieces of cartilage and bone with a diameter of 6-8 mm and a length of 15 mm from the non-load-bearing region of the joint and transferring them to the damaged area in the load-bearing region. This technique is used for cartilage damage smaller than 4 cm. It is most commonly applied to the knee and ankle joints. The procedure can be performed arthroscopically, that is, by the closed method. The most important advantage is that a tissue with the structure of normal cartilage is transferred to the damaged area. In other words, the cartilage placed in the damaged area is not the healing cartilage, but the original joint cartilage. The disadvantages are that a limited number of tissue transplants can be performed and normal cartilage in another part of the joint is sacrificed for transplantation. In very large damage, tissue may also need to be taken from the opposite knee joint sometimes, which is intact. Due to the nature of the technique, only 70% of the damaged area can be filled with the transplanted cartilage, and the area between the transplanted cylinders heals with a cartilage-like repair tissue. This technique is generally more successful in minor cartilage damage. It may be difficult to establish the normal shape of the joint in areas of major injury. The postoperative period is similar to the micro-fracture method.
Cartilage Transplantation
In recent years, the most researched and scientifically developed area is cartilage transplantation. In this technique, a few mm of cartilage tissue in the form of chips is removed from the non-load-bearing part of the joint in the area where cartilage damage is detected by arthroscopy. This tissue is processed in a laboratory environment under sterile conditions and is reproduced by multiplying the cartilage cells in it. The new cartilage cells formed after this procedure, which lasts for a few weeks, are transplanted to the damaged area by open surgery. In cartilage transplantation techniques, these cells are injected under a membrane-shaped tissue taken from the tissues around the knee and sutured to the damaged area.